In the past few years, the intraoral scanner market has become more competitive than ever before, with multiple companies introducing cheaper alternatives for less than USD 20,000. How do they perform in a clinical environment? Are more affordable scanners as good as the expensive ones? Let’s compare five scans of the same prep, scanned by the same operator using one high-end IOS and four affordable scanners.
The increasing competition in the dental market has changed the status quo in the past few years. More CAD/CAM systems have become open, and the focus is shifting towards software and app development, all while subscription fees are being decreased/removed.
The intraoral scanner prices have gone down significantly, effectively reducing the financial obstacles, and many dentists worldwide are now considering getting their first scanner.
As anything labeled “cheap,” even medical devices won’t avoid having their quality questioned. In our reviews, we often mention how these scanners feel and look. When it comes to accuracy, the discussion becomes more complicated, and the question of trueness and precision has to be answered by researchers. We share our objective and unbiased experience with daily use in clinical workflows with you: real-life patients and real-life cases.
We have already tested most of these scanners, and new IOS are sent to us almost every month. Besides the standalone reviews of each scanner, we summarized our experiences in our IDS 2021 review.
One Prep, Five Scanners
As it’s the case with all of our iDD Compares posts, we present you with the same case as scanned by the same operator using multiple different scanners. In this particular case, I used these scanners:
- TRIOS 4 by 3Shape
- S6000 by DentaLink
- Heron IOS by 3DISC
- i700 by Medit
- DL-206P by Launca
The last four scanners are pretty affordable, all within a USD 13-20k price range, while the cheapest configuration of TRIOS 4 starts at USD 34,000. 3Shape scanners are generally regarded as quality and accurate devices, with studies backing these claims, which is why we used this scanner as a baseline for others.
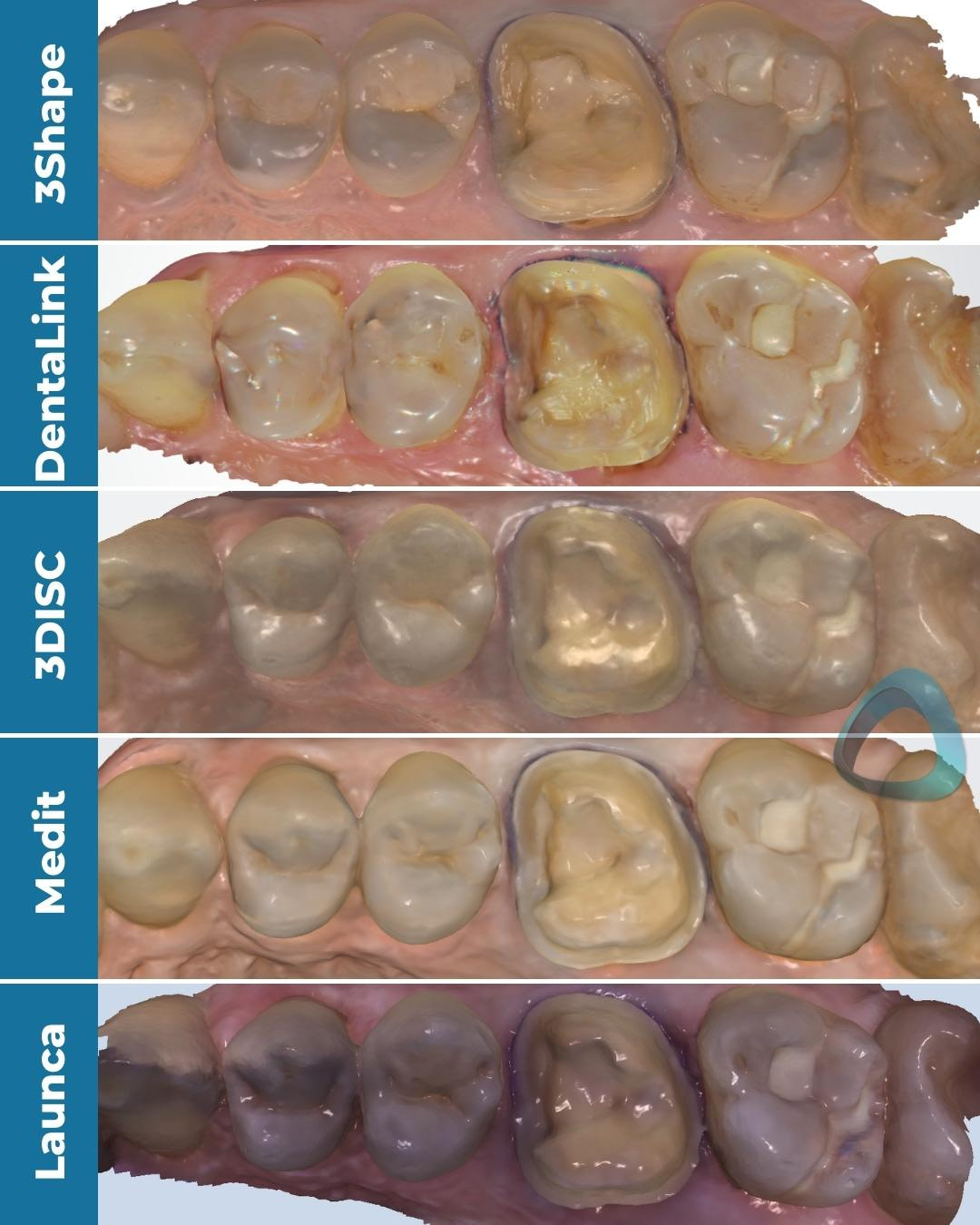
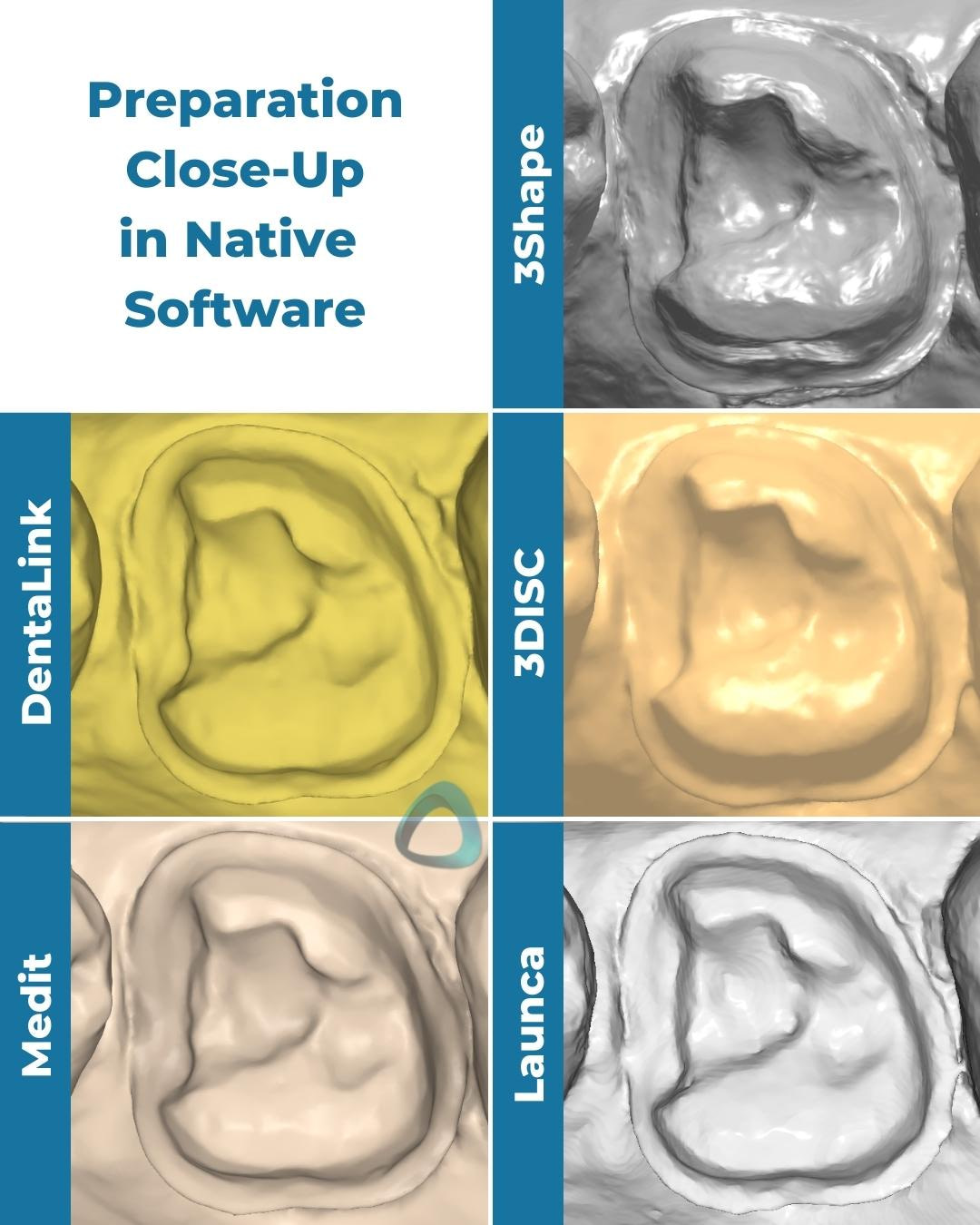
We show the scans both in color and monochrome as previewed in their native software, which should give you a clear idea of how these scanners capture colors and textures. The color rendering helps identify the margin, but the monochrome rendering is crucial for assessing the quality of the captured scans, especially the margin.
In the following pictures, you can see how each scanner handles these previews, which becomes important if their software has an option to marginate before sending the scans to a dental lab.
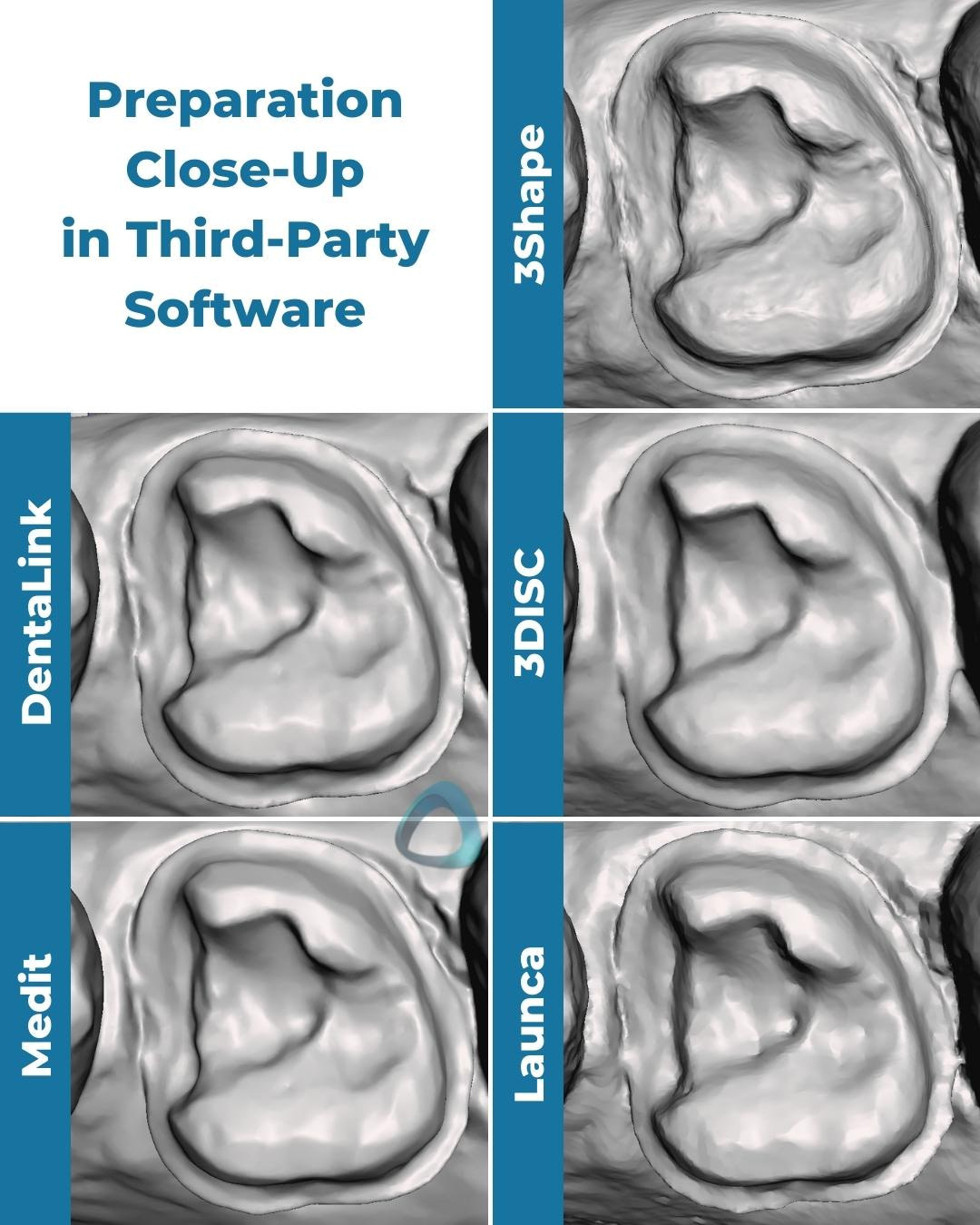
Monochrome Presentation in Third-Party Software
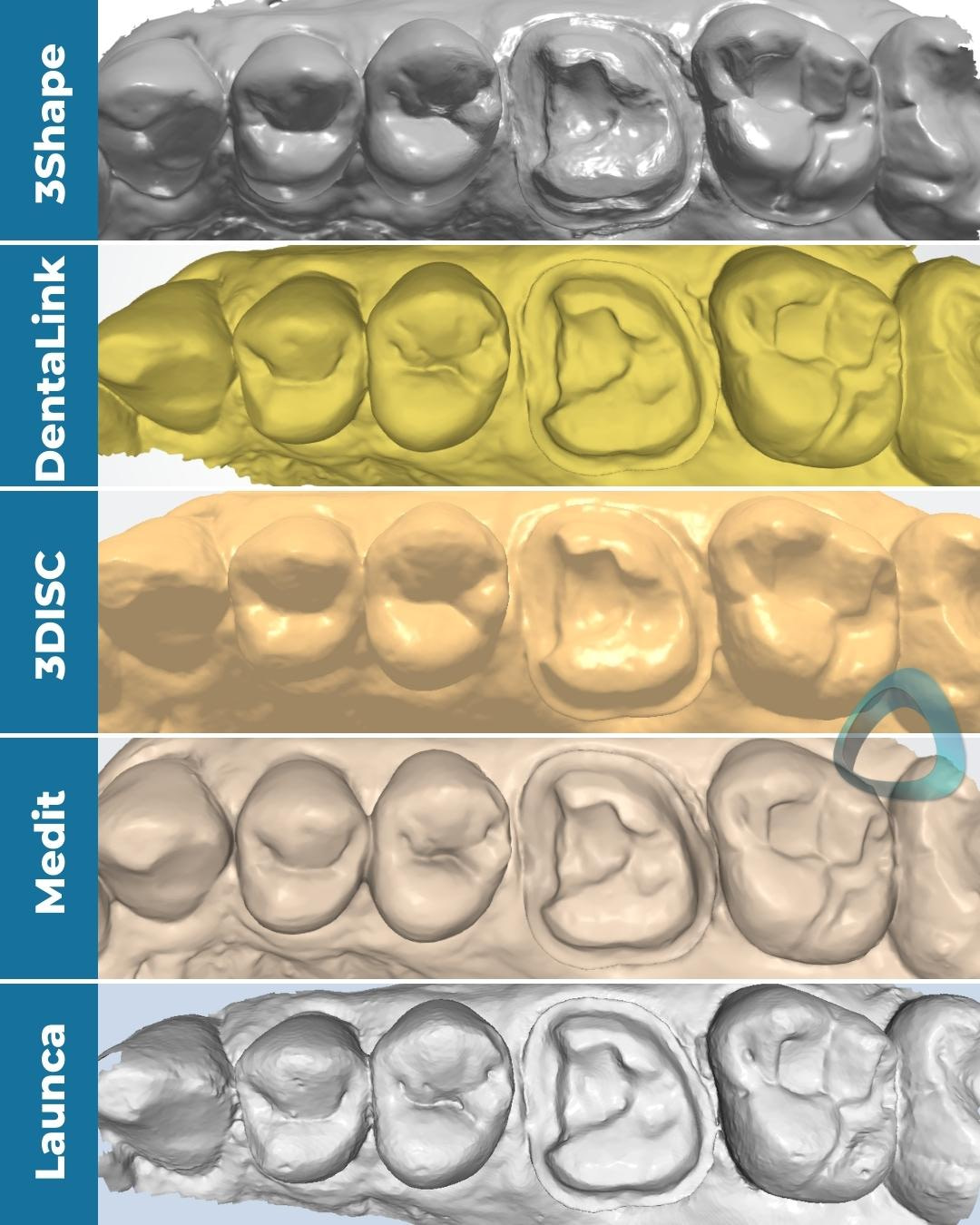
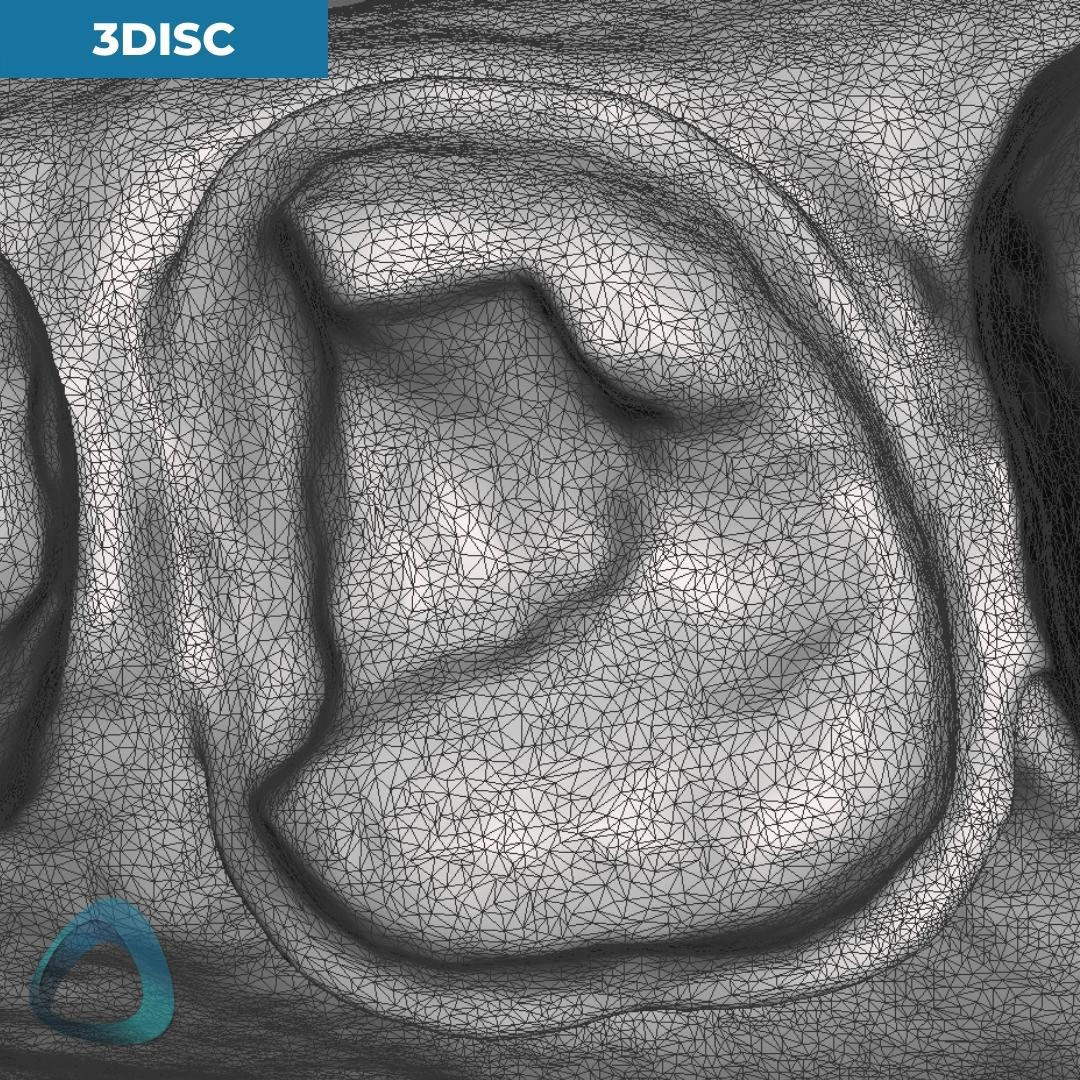
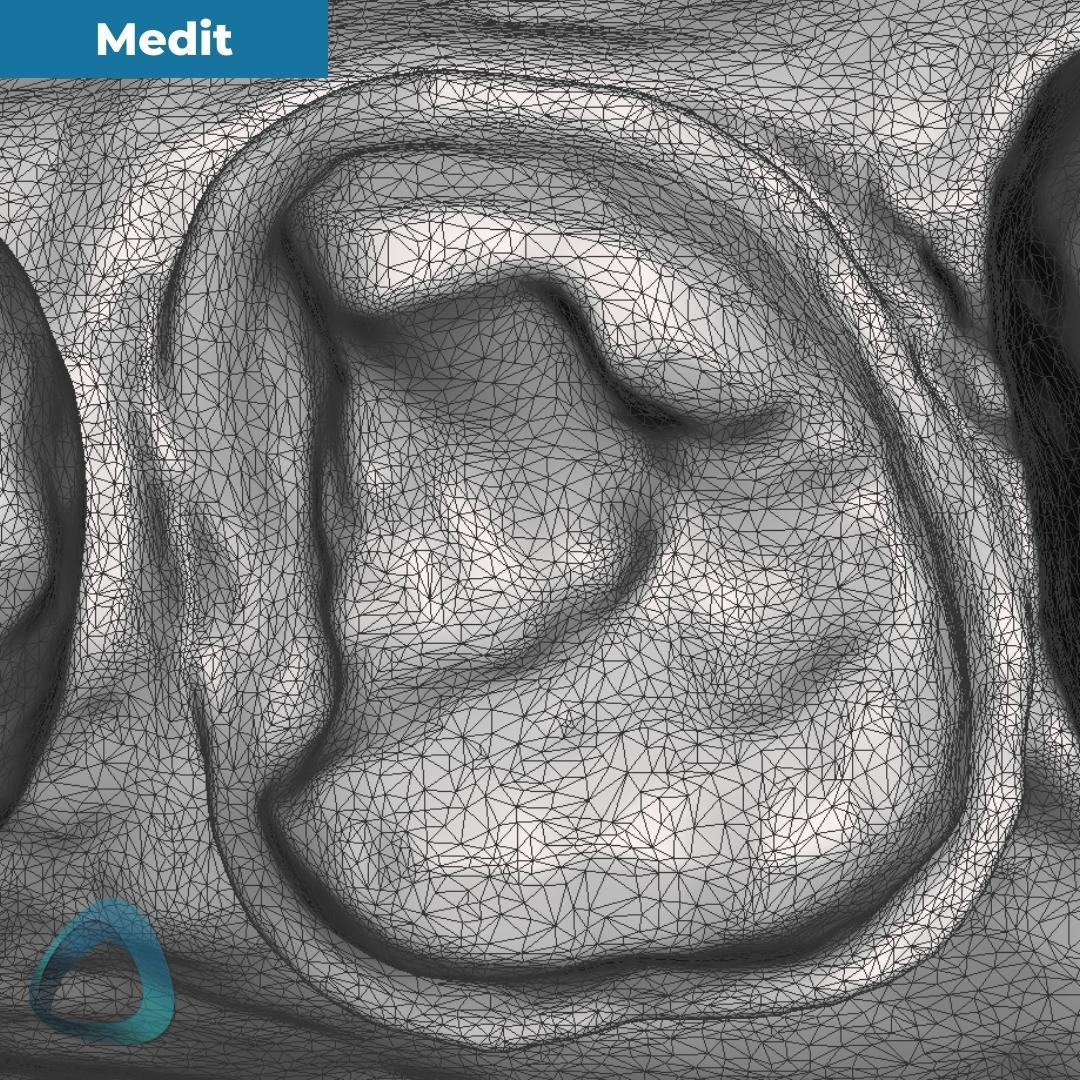
We also exported these scans in an STL format and previewed them in third-party software (Meshmixer by Autodesk) with and without the tessellated mesh. All the scans were exported with their default settings, and the Medit i700 scan was NOT captured in HD.
Showing the files in third-party software helps us have a level playing field. The scans can’t hide behind the software’s rendering, and it gives you an idea of what you or your lab would see in CAD software such as exocad’s DentalCAD or 3Shape’s Dental System. Considering that most dentists will use these IOS primarily as an impression-replacement tool, it’s crucial to assess the exported data.
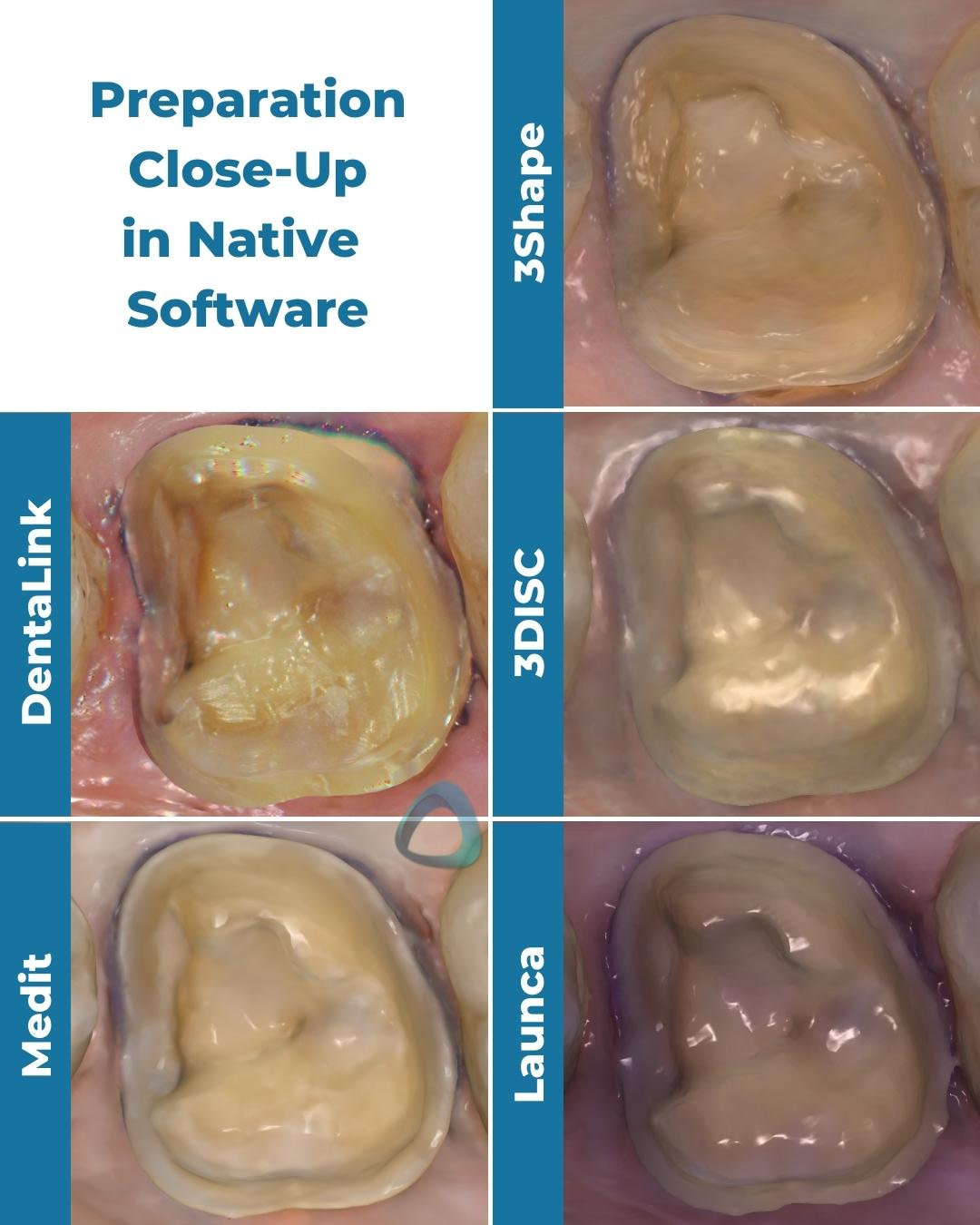
It also makes the differences between IOS more prominent, or in some cases, it proves that the difference is not huge at all. The most noticeable difference in this particular set of scans is in the interproximal margin areas, which is equigingival. Scanners generally struggle with equi or subgingival preparations (but can be managed with proper tissue and moisture control), and you can see the margin is easier to read with some scanners than others.
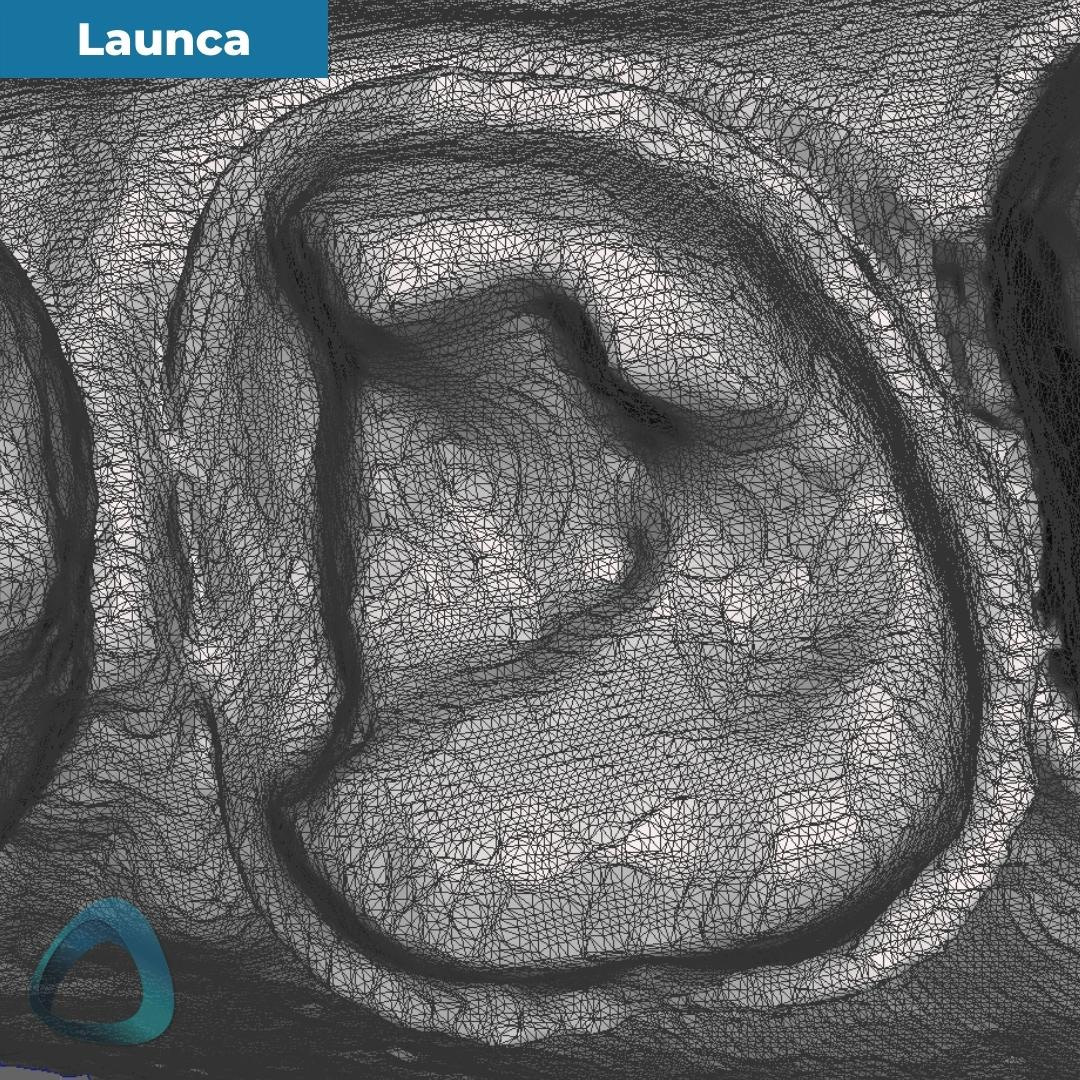
It also highlights that Launca has more difficulty around the palatal portion of the margin, and the margin in this area seems to be deformed due to enamel translucency.
Modern IOS devices use a light source, and to scan correctly, they need the projected light to bounce back off the surfaces. The data is not captured accurately if the light doesn’t bounce back and goes through the surface instead.
This is why older scanners used sprays to cover the oral structures with a fine layer of powder, making them effectively opaque. Most modern intraoral scanners have solved this issue and do not require a spray anymore but can still have problems with translucent surfaces.
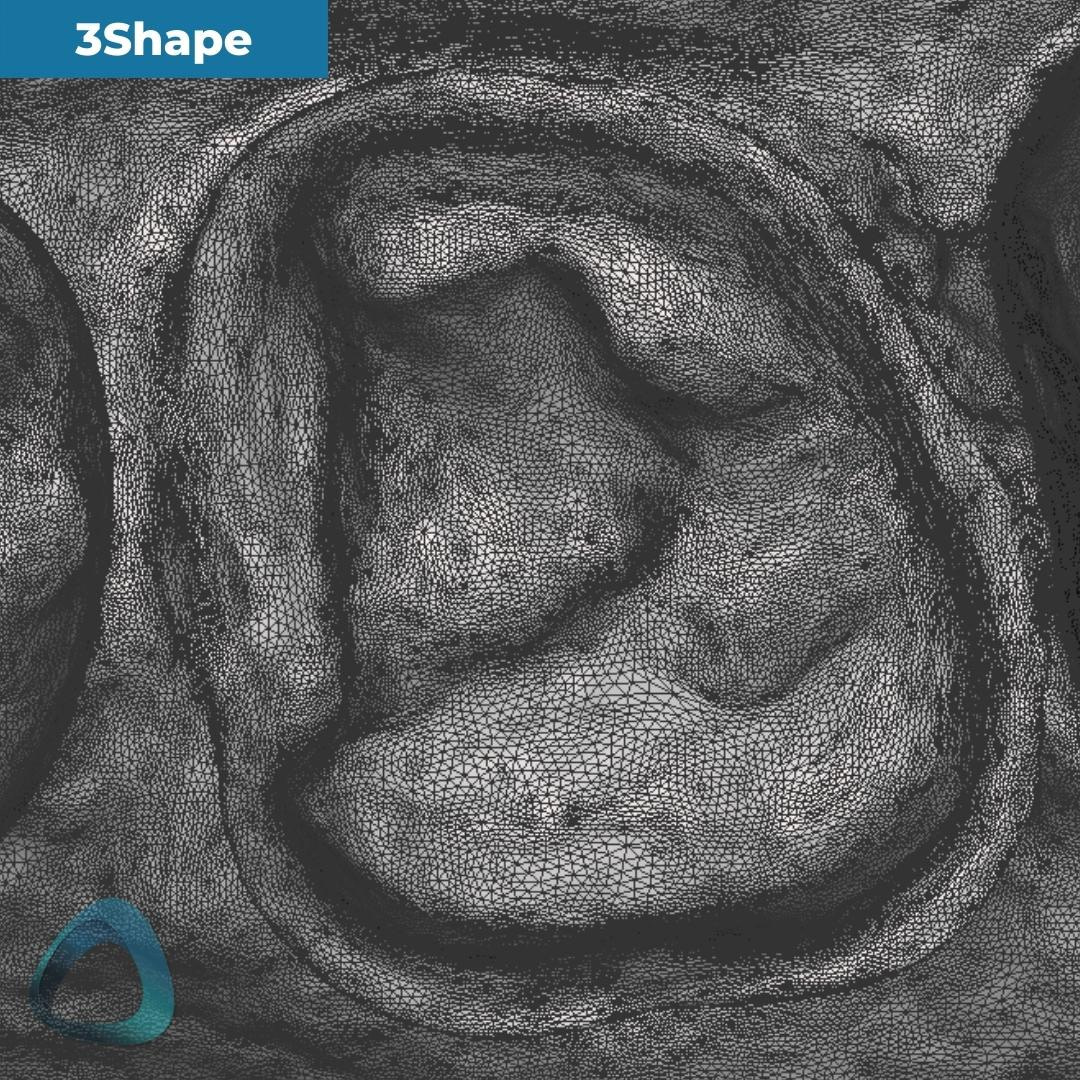
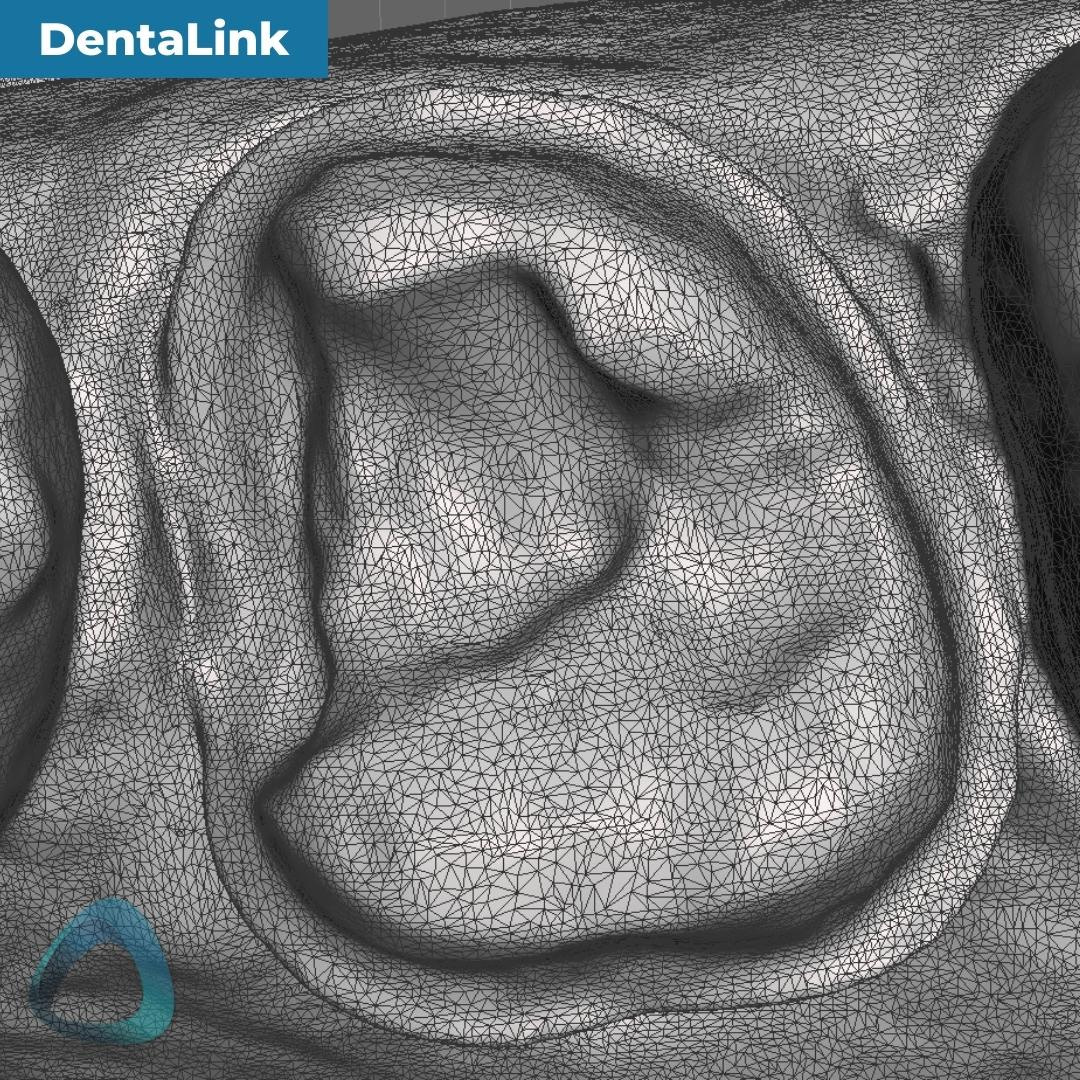
The tessellated mesh provides us with a good insight into how the data was captured and stitched together. As you can see in this particular case, Launca DL-206P’s finer tesselation doesn’t necessarily mean a ‘better scan.’
Conclusion
The bottom line is that not all scanners are created equal. There seem to be noticeable differences in the quality of captured data, which might result in compromised margin detection.
There are also apparent differences in how the software of each scanner renders the images. Whether or not these findings are clinically significant is a topic of debate, mainly because regardless of what the scanner can pick up, there are also limitations in the milling/production process. A lot more research needs to be carried out testing all these new scanners coming on the market.