As digital dentistry continues to evolve, so too do the components we use in our restorative workflows. One area that has seen significant innovation is prosthetic screw design for full-arch implant restorations.
Historically, many clinicians and labs relied on small, straight “pros-screws” that worked well enough for older workflows. However, with the rise of monolithic zirconia and photogrammetry-based full-arch workflows, these legacy screws introduced certain risks, such as fracture or misfit, prompting the development of new-generation screw designs (e.g., “Powerball,” “Vortex,” and “Rosen”).

Some practitioners don't have an intraoral scanner, while others are masters of photogrammetry and immediate load All-on-X digital workflows. This knowledge gap means labs often handle screw selection, as many dentists rely on the lab’s expertise to choose the most appropriate screw for a given full-arch case. Or have no idea about different options.
In my experience, this entire topic is poorly understood. So in this article, we'll explore the evolution of prosthetic screws, examine modern designs, and discuss their practical implications for both clinical and laboratory workflows.
I collaborated with Lachlan Thompson, owner of Omni Dental, on this piece. Lachlan has over 20 years of experience in dental technology and has built one of the most respected full-arch laboratories in Australasia, operating two facilities in Western Australia and Melbourne. His team has been at the forefront of complex full-arch restorations, pioneering rapid milling workflows as early as 2013 and adopting photogrammetry systems early, when most labs were still building verification jigs. His clinical insight was invaluable.
Below, we explore why these new screws matter and how they solve critical problems in modern full-arch implant therapy.
A Brief History - Where We Started
The evolution of prosthetic screws mirrors the broader evolution of full-arch restorations. Early implant dentistry used floating chrome bars and PFM (porcelain-fused-to-metal) solutions. Materials progressed from basic acrylics through Montreal bars and eventually to modern zirconia. And through all of this, the screw changed very little.
Traditional prosthetic screws were relatively simple: straight walls, basic engineering, and a design philosophy built around older restorative approaches. They worked well enough for what they were designed to do. But two major shifts changed everything.

First, the rise of ceramic materials, particularly zirconia, demanded better stress distribution. Ceramics respond to occlusal forces very differently from metal, and straight-walled screw seats with sharp edges create exactly the kind of stress concentration points that lead to fractures in monolithic frameworks.
Second, there has been a strong push to eliminate titanium bases (tibases) in digital workflows. Cemented tibases introduce potential debonding issues, additional tolerance stacking, and reduced accuracy over the long term. The industry has responded by engineering screws that allow frameworks to be milled directly onto multi-unit abutments (MUAs), bypassing the tibase entirely.
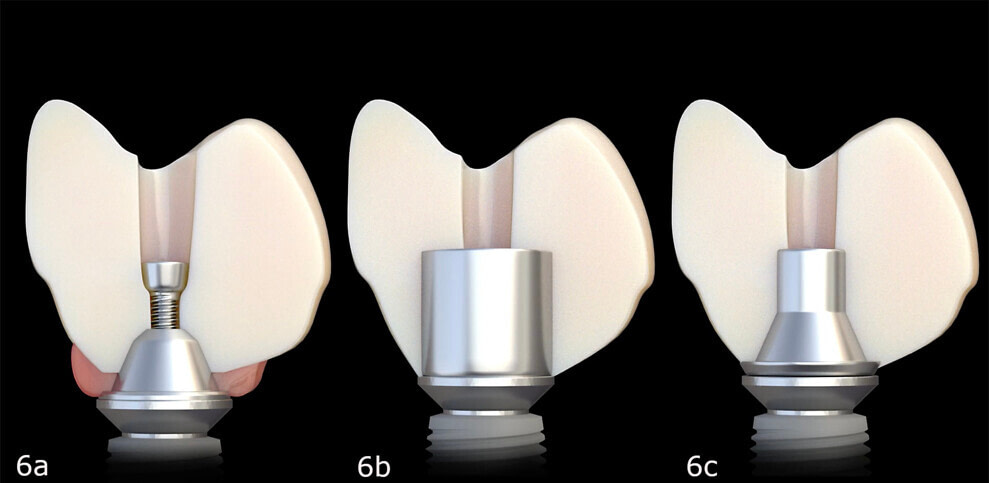
Three methods of attaching zirconia restorations to implants.
A) Conventional multi-unit abutment. B) Titanium bar. C) Titanium base. Source Image
An early pioneer worth acknowledging here is Nobel Biocare's Procera system. Their Procera abutments featured a bevelled screw seat specifically designed to disperse stress outwards, combined with a longer shaft to increase the material thickness between the screw seat and fixture. That concept, stress redirection through geometry, is the foundation on which modern screw designs have been built.


The problem with older screws? Some provided as little as 0.5mm of material above the abutment. Under heavy bite forces, the restoration could pull through or fracture around the screw seat. That is simply risky in a full-arch case.
The Direct-to-MUA Evolution
Before diving into the screws themselves, it is worth understanding the broader workflow shift that necessitated this conversation. The growing adoption of direct-to-MUA techniques, where a framework is fabricated to seat directly onto the MUA without any intermediate tibase, has created demand for a completely different class of prosthetic screw.
Traditional screws were never designed for this. The new generation, including Powerball, Vortex, and Rosen screws, were built specifically for this workflow. Each uses some form of conical screw geometry to prevent loosening and achieve the kind of direct retention that eliminates the need for cementation altogether.
Key Evolution Factors:
- Older screws create stress fractures in monolithic materials due to the straight edges.
- Ceramic materials requiring improved stress distribution
- They often offer insufficient thickness above the abutment, increasing pull-through risk.
- Desire to eliminate titanium bases in digital workflows
- Push for greater accuracy and reduced cementation issues
The question becomes: which design is right for your cases? Let's go through each one.
Modern Screw Designs
New-generation screws, such as Powerball, Vortex, and Rosen, are engineered to address issues of stress distribution, tibase misfits, and milling complexity.
Key innovations include rounded seats that distribute occlusal forces more evenly and designs that enable labs to mill frameworks directly onto multi-unit abutments, thereby eliminating traditional tibases.
Summary of new-generation screw advantages
- Modern screws often have a spherical or beveled seat for improved stress distribution in zirconia or PMMA.
- They generally allow direct-to-abutment workflows, avoiding the cementation of tie-bases.
- Many are designed with milling-friendly geometry, making fabrication more efficient and accurate.
Below are the most common new-generation screws that digital-focused labs work with. Each design offers distinct pros and cons based on geometry, ease of milling, and clinical usability.
Powerball Screws
Currently one of the most widely used options in the market, Powerball screws are named for their distinctive ball-shaped screw seat. That spherical geometry is the key design feature, and it exists for a specific reason: to distribute occlusal forces more evenly through the prosthesis rather than concentrating them at a single contact point.
The Powerball's geometry also has a practical manufacturing benefit. Because the ball shape mirrors the geometry of standard milling burs, labs can machine the screw seat from the occlusal aspect using a straightforward top-down milling approach. No specialized T-burs required, no milling from multiple angles. This simplifies fabrication considerably and keeps tooling costs manageable.
One notable consideration is their taller profile, which extends approximately 2mm above the multi-unit abutment, potentially impacting prosthetic space requirements.

Advantages
- Uniform stress distribution - the spherical shape evenly spreads occlusal forces within zirconia or PMMA frameworks, reducing fracture risk.
- Top-down milling - their shape is based on the geometry of common milling burs, so labs can easily machine the screw seat from the occlusal aspect. This process avoids specialized T-burs or milling from underneath.
- TiBase elimination - since the framework is milled directly to the multi-unit abutment, there is no need to cement a TiBase, potentially improving overall accuracy.
Drawbacks
- Profile height - Powerball screws extend approximately 2mm above the MUA. This can be a real challenge in cases with limited restorative space, particularly in FP-1 type restorations
- Larger access hole - the screw channel is typically bigger than alternative designs, which in some cases compromises material thickness around the channel
Rosen Screws
These screws feature a distinctive long taper design that brings both advantages and challenges to the restoration process.
The advantages of Rosen screws are significant. Their small head size requires less prosthetic space, making them suitable for cases with limited vertical clearance. The design provides excellent torque characteristics during seating, which can help ensure proper prosthesis fit. These screws work particularly well with polymer materials, offering reliable retention. The increased surface area of the taper design can potentially provide better retention of the prosthesis.
However, there are several important drawbacks to consider. The tapered design can be particularly challenging to seat when the prosthesis is misaligned, potentially leading to fit issues. There is also a risk of cold welding, which can make prosthesis removal difficult if needed. From a manufacturing standpoint, these screws require more complex milling procedures. When used with ceramic materials, there are concerns about stress concentration at certain points of the taper.

Advantages
- Strong torque retention - the deep taper rarely comes loose once torqued, ensuring a secure fit
- Small screw head - rosen screws often have a narrower head, which means a smaller screw channel and less intrusion on prosthetic design
- Strong lateral wall retention once torqued correctly
- Works well with polymer materials
Drawbacks
- Potential for cold welding and snapping - morse tapers can become difficult to retrieve if minor misalignment causes tension; screws can seize or fracture.
- Milling complexity - the taper geometry often requires specialized T-burs, which can cost around USD $350 each and require milling from specific angles
- Stress concentration - in ceramic materials, the taper design can concentrate stress at certain points in a way that the rounded geometries of Powerball avoid
Vortex Screws
Representing a hybrid approach, Vortex screws combine elements from both Powerball and Rosen designs to create a unique solution. The design incorporates both ball and taper elements, aiming to capture the benefits of both approaches.
Manufacturing these screws requires specific considerations, particularly the need for underside milling in many cases. Despite this additional complexity, the design offers excellent stress distribution while maintaining a reasonable screw channel size that doesn't overly compromise the prosthetic design.

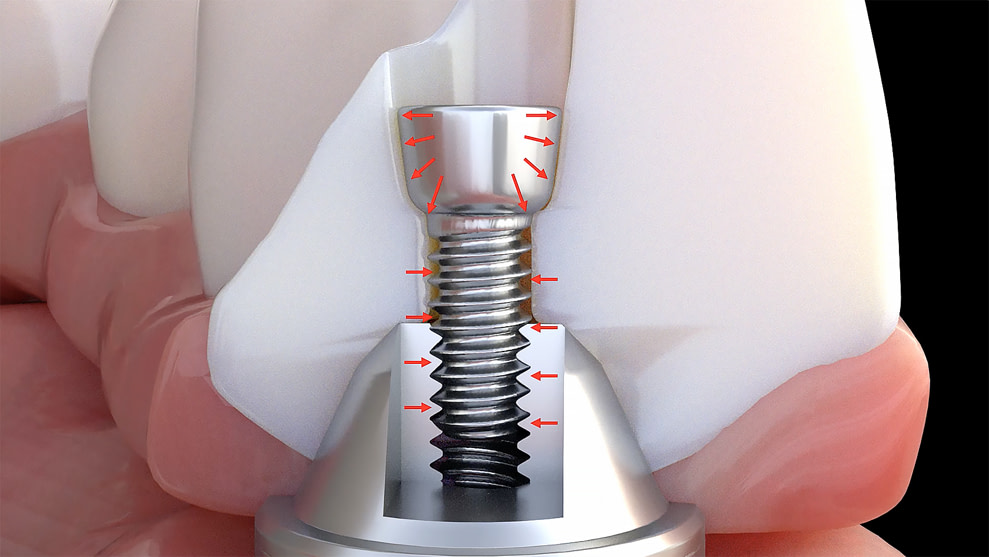
Vortex LA VIS screw attached directly to the multi-unit abutment, allowing increased thickness of zirconia based on available interocclusal space. (Image: Danny Domingue). Source Image.
Advantages
- Curved seat for better stress relief - though partially tapered, the design includes a rounded area that minimizes stress points.
- Slightly smaller head - vortex screws can be less bulky than original Powerball designs, which some clinicians find preferable for aesthetics and easier finishing.
Drawbacks
- Undercut milling challenges - if the implant angle is steep, labs may need to approach the screw seat from underneath using T-burs. These burs are fragile and expensive to replace.
- Precise alignment - the partial taper still demands precise alignment in both digital design and mouth insertion to avoid internal tension.
A Potential Problem With Conical Screws
Here is something that does not get discussed enough. Powerball, Vortex, and Rosen screws share a common design principle: they are all conical. And that creates a mechanical reality that is worth understanding.
Conical screw designs rely on the assumption that the screw will self-center within the MUA connection geometry. In a single-implant case, that works fine. But in a full-arch restoration seated across multiple implants, perfect alignment across all MUA connection geometries simultaneously can be difficult. Even small deviations in milling or implant angulation mean the conical screw is not perfectly centered, and that introduces internal mechanical stress to the restoration from the moment it is seated.
Alternative Designs - Tri Matrix, DESS and Badger
It's worth noting that new designs continue to emerge in the market. For example, the Tri Matrix screw features an interesting combination of a flat bottom and a rounded top design. While this approach differs from the ball-shaped trend seen in other modern designs, it represents another attempt to optimize stress distribution. However, as with many newer options, market adoption and long-term clinical performance data are still developing.

There are also a few other screws to consider - DESS has taken a different approach with its Flat Seat Screw, which uses a flat rather than conical seat geometry. Their testing shows the flat seat achieves higher preload forces than conical designs even at lower torque values (their data showed superior performance at 15Ncm compared to the Rosen screw at 20Ncm), and the flat seat design accommodates divergences in screw hole milling more predictably than conical alternatives. The seat is also 1mm thick, 2.5 times thicker than older screw designs. The DESS Flat Seat also uses a Torx socket and supports angulated screw channels up to 25 degrees. Once again, this is manufacturer-reported data, and independent, peer-reviewed evidence comparing these designs in long-term clinical settings remains limited. That said, the mechanical argument for a flat seat in multi-implant frameworks is logical and worth considering.

Another newer design worth discussing is the Badger Screw, which takes a different approach again. Instead of relying on a conical or flat seat, it utilizes a concave profile aimed at increasing vertical clamping force while reducing stress concentration within the prosthetic. I hear a lot of people in the USA raving about this screw type as well.

From a mechanical perspective, the idea is interesting. A concave interface may allow the screw to maintain more consistent contact under load, potentially improving preload retention and reducing the likelihood of loosening. The design is also marketed as enabling a smaller screw channel, which helps preserve prosthetic strength by removing less material. Additionally, manufacturer data suggests the Badger Screw achieves high clamping forces (reported >300N in zirconia) while aiming to minimize prosthetic stress, likely through its geometry and load distribution strategy.
However, as with many emerging screw designs, most of the available data is manufacturer-driven, and independent clinical validation, particularly in long-term full-arch cases, is still limited.
Technical Considerations
Manufacturing Impact
The choice of screw design can significantly impact manufacturing processes, particularly in milled restorations.
Powerball screws have been specifically engineered to enable straightforward top-down milling with standard tools, significantly simplifying the manufacturing process. In contrast, Vortex and Rosen designs often require specialized tooling, such as T-tools that can cost around $350 each, and may need milling from multiple angles.
The complexity of manufacturing varies significantly between designs. For example, some screw seats require milling from the underside of the restoration, which necessitates specific tool access angles and can increase production time.
Material thickness requirements also vary significantly between designs. Traditional screws left as little as 0.5mm of material above the abutment. Modern designs can require up to 2mm. That directly influences your prosthetic design options and your restorative space planning.
Manufacturing Considerations:
- Tool costs and specialization requirements
- Access angles for milling
- Production time implications
- Material thickness requirements
- Impact on prosthetic design
Stress Distribution
Modern screw designs, particularly those featuring curved or ball-shaped elements, aim to distribute forces more evenly through the prosthesis. This is especially important when working with ceramic materials, which are more susceptible to stress concentrations. The curved surfaces help to eliminate sharp angles where stress can concentrate, potentially reducing the risk of material failure under load.
Clinical Implications
While there's currently limited scientific evidence demonstrating the clinical superiority of any particular design, practical experience and clinical feedback provide valuable insights.
For example, while Powerball screws offer theoretical advantages in stress distribution, some clinicians report challenges related to their larger screw channel size and increased height requirements. Conversely, while Rosen screws may pose manufacturing challenges, they can perform well in clinical settings with limited space.
Several practical considerations influence screw selection. The ease of seating of the prosthesis can vary significantly across designs, with some requiring more precise alignment than others. The size of the screw channel directly impacts prosthetic design options and aesthetics. Available vertical space for the restoration must be carefully considered, as some modern designs require more height than traditional options. The choice of restorative material, whether ceramic or polymer, may also influence which screw design will perform best.
Laboratory Perspective
From a laboratory standpoint, several important factors influence screw selection:
- The manufacturing capabilities and equipment available in the laboratory will often dictate which screw designs can be efficiently produced.
- Material preferences and their compatibility with different screw designs play a crucial role in the decision-making process.
- Workflow efficiency considerations, including milling time and complexity, can impact production schedules and costs. Tool wear and replacement costs must be carefully considered, particularly with designs requiring specialized tooling.
- Stock management becomes more complex when multiple screw designs must be maintained for different cases and clinician preferences.
Key Laboratory Considerations:
- Manufacturing capabilities and equipment limitations
- Material compatibility and preferences
- Workflow efficiency and production time
- Tool wear and replacement costs
- Stock management complexity
- Clinician preferences and requirements
Conclusion
The prosthetic screw has come a long way from the simple straight-walled designs that underpinned earlier full-arch workflows. Modern designs address real clinical problems: stress fractures in monolithic ceramics, the elimination of tibases, and the push for greater passive fit accuracy.
That said, no single design is perfect for every case. Powerball offers genuine manufacturing advantages and good stress distribution, but demands adequate restorative space. Rosen gives you a smaller profile at the cost of milling complexity and cold-welding risk. Vortex sits between them but does not fully resolve either problem. And the emerging flat-seat approach challenges the conical paradigm entirely, with a mechanical rationale worth paying attention to.
There is no universal right answer here, and anyone telling you otherwise is simplifying the decision. The right screw for a given case depends on a combination of clinical, material, and laboratory factors. That said, as direct-to-MUA workflows become the norm rather than the exception, the conversation around screw design will become far more prominent in the implant literature. We are early in that conversation.
If you are the clinician placing these restorations, take the time to understand what your lab is using and why. If you are the lab, make sure you are matching the screw to the case rather than defaulting to a single design across the board.
Thanks for reading. If you have any input, please leave it in the comments below.
A big thanks again to Lachlan Thompson, owner of Omni Dental, for collaborating on this article. Lachlan brings over 20 years of dental technology experience and oversees a team of 50+ technicians specialising in complex implant prosthetics and digital workflows.


